Today
was slow again. Chores and a few
technician appointments took up most of the day. We had two new patients in the recovery room:
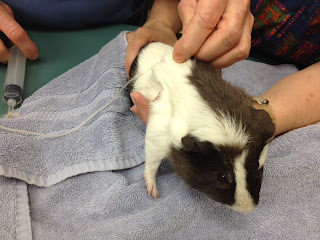
a Pug named Charlotte who was recovering from her pyometra surgery, and a
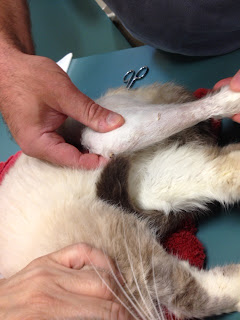
Persian cat named Frisco who was having seizures and heart problems. Both of them went home during the early
afternoon. In addition, during the later
afternoon, we had an emergency that came rushing in; a six year old Lab/Dane
mix named Scruffy who was seizing, twitching when he wasn’t seizing, having bloody diarrhea, foaming at the mouth,
etc. Catherine and one of Scruffy’s
owners rushed him into the back area where we work on a blanket, and Dr. Kris
and Dr. Lou began rushing around trying to figure out what was wrong with him
and what to give him (medicine-wise) to calm him down. Dr. Lou started by giving him valium to stop
the seizing (which it did, and nearly as soon as she injected it), and Dr. Kris
went to talk to the family to see what they knew and try to figure out what
exactly was going on. When she came
back, she said that Scruffy’s problem could be a number of things and she
really didn’t know what it could be. Heat stroke, Isoloma (a plant that causes
problems when ingested), poisoning (from a palm, gum, etc.), bacterial growth, etc.—they
didn’t know. He was still breathing
heavily, and he had a blood sugar of 20 mmol/L (extremely low), a heart rate of 180 BPM, and a temperature of 104 degrees. Dr. Lou had me give him Dextrose solution so his
blood sugar could rise, Ampicillin to fight off any bacteria in his respiratory
tract, stomach, and/or urinary tract, and IVs and sub-q fluids to hydrate him
and cool him down (after a little while his blood sugar rose to 105 mmol/L, and
his temperature went back down to 98 degrees).
While the doctors were trying to figure out what was going on, I sat by Scruffy
for over an hour and a half—making him comfortable with blankets and pillows,
stroking his head, wiping his saliva and tears, giving him the fluids and
antibiotics the doctors asked me to give him, etc. Scruffy was in a lot of pain (as I said, he was
crying), and he was whining and crying out the entire time. I felt terrible for him… and I felt even worse
because I didn’t know what I could do.
Since I’m not a doctor, there’s nothing I really could do; that’s why I was sitting by him and taking care of him,
since that was the only thing in my power that I knew I could do for him. I absolutely hate the feeling of
helplessness, and that’s how I felt while I was sitting with him. But at the
same time, even though I feel awful for the animal during times like these, it’s
also these times that I remember why I want to become a Veterinarian. I absolutely adore these animals, and I want
to be able to help them. I don’t want
them to be in pain or suffering in any way; I want them to be healthy and
happy.

Frisco the Persian. He was a bit cranky.
Charlotte the Pug.
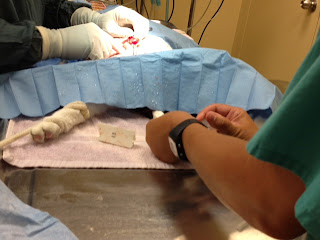
Scruffy when he first came in; Dr. Lou was injecting the Valium to get him to stop seizing (Catherine was holding him fairly still so Dr. Lou could inject it without hurting him or missing the vein).
Scruffy when he started to calm down.
Around the time that Scruffy came in, it also
started to become really busy; the doctors were starting to have appointments
scheduled so lots of animals were starting to be brought to the back and the
doctors were trying to do the appointments as well as take care of Scruffy. After taking care of a couple appointments,
Dr. Kris went back in to talk with the family again. When she came back, she had a pretty good
idea that something had poisoned Scruffy—the lady has a palm plant in her house
(which she had also just trimmed yesterday, so maybe he ate a piece off the
floor rather than off the plant), and Scruffy also likes to go through one of
the son’s garbage bins (in his room), which he throws gum into a lot. Therefore, Dr. Kris and Dr. Lou believe that
he may have ingested gum or part of the palm plant. They gave him some antibiotics and some
charcoal to make him regurgitate, and Nancy and I moved him to the corral so he
could rest there and let the medicine and charcoal do their jobs. After this incident I went home for the day,
and I hope he’s doing okay. I’ll have to
check on him again tomorrow!